Nigerian government doing a poor job on water/sanitation and health care, citizens say
- Apr 28, 2022
- 9 min read
Afrobarometer Dispatch No. 389 | Raphael Mbaegbu and Chukwudebe Nwanze
Summary
The COVID-19 pandemic has worsened problems that were already bedeviling Nigeria’s health system, including run-down or inadequate medical equipment, underpaid and unmotivated medical staff, and unequal access to health care (Andolu Agency, 2020; Pulse Nigeria, 2020). The World Health Organization has labeled Nigeria a human resources for health (HRH) crisis country (Global Health Workforce Alliance, 2020).
The pandemic has also highlighted citizens’ inadequate access to water and sanitation facilities. Nigeria has pledged its commitment to meeting Sustainable Development Goal (SDG) 6, which is to “ensure access to water and sanitation for all” by 2030. But the National Longitudinal Phone Survey (NLPS) on the socio-economic effects of COVID-19 shows that many households in Nigeria do not have sufficient access to soap and water for handwashing and that there is low adherence to hygiene protocols (National Bureau of Statistics, 2020; Premium Times, 2020).
The most recent Afrobarometer survey in Nigeria, conducted in early 2020, shows that even before the COVID-19 pandemic, majorities of citizens reported going without needed medical care and clean water at least once during the previous year. Nigerians give the government low marks for its performance in providing water and sanitation services and improving basic health services.
Afrobarometer surveys
Afrobarometer is a pan-African, nonpartisan survey research network that provides reliable data on African experiences and evaluations of democracy, governance, and quality of life.
Seven rounds of surveys were completed in up to 38 countries between 1999 and 2018. Round 8 surveys in 2019/2021 are planned in at least 35 countries. Afrobarometer conducts face-to-face interviews in the language of the respondent’s choice with nationally representative samples.
The Afrobarometer team in Nigeria, led by NOIPolls, interviewed 1,599 adult citizens in January-February 2020. A sample of this size yields country-level results with a margin of error of +/-2.5 percentage points at a 95% confidence level. Previous surveys were conducted in Nigeria in 1999, 2002, 2005, 2007, 2008, 2012, 2014, and 2017.
Key findings
▪ Only three in 10 Nigerians (29%) live in zones served by a piped water system, and even fewer (18%) have sewage systems their homes can access. Two-thirds (65%) live within walking distance of a health clinic.
▪ Fewer than one in 10 citizens (8%) get their water from pipes in their dwelling place or compound. For most (65%), the main source of water is boreholes or tubewells.
o Three in 10 respondents (30%) do not have a toilet or latrine in their home or compound.
▪ Close to six in 10 Nigerians (57%) say they went without enough clean water at least once during the previous year, a 17-percentage-point increase compared to 2017.
▪ Two-thirds (65%) of Nigerians say they went without needed medical care at least once during the previous year, a 22-percentage-point increase since 2014.
▪ Among respondents who had contact with a public health facility during the previous year, about four in 10 (38%) report difficulties in obtaining care, and two in 10 (21%) say they had to pay a bribe.
▪ Only about one-third (36%) of Nigerians say the government is doing “fairly well” or “very well” on improving basic health care, and even fewer (27%) approve of the government’s performance in providing water and sanitation services.
Presence of infrastructure
During the survey, Afrobarometer’s field interviewers observed and reported the presence of key basic infrastructure in each enumeration area they visited. The fieldworkers found that while eight in 10 respondents (81%) live in areas with boreholes or tubewells, only three in 10 (29%) live in zones served by a piped water system (Figure 1). Even fewer (18%) are in zones with sewage systems, while two-thirds (65%) live within walking distance of a health clinic.
Rural residents are significantly less likely than their urban counterparts to have access to water, sanitation, and health infrastructure. The largest disadvantage (28 percentage points) concerns health clinics, but double-digit gaps exist for each of these types of infrastructure.
Figure 1: Presence of health, water, and sanitation infrastructure | by urban-rural location | Nigeria | 2020

Survey enumerators were asked to record:
Are the following services present in the primary sampling unit/enumeration area: Piped water system that most houses can access? Sewage system that most houses can access? Borehole or tubewell?
Are the following facilities present in the primary sampling unit/enumeration area or in easy walking distance: Health clinic (private or public or both)?
(% “yes”)
Access to water
Boreholes and tubewells are the most common sources of water for Nigerians (cited by 65%) (Figure 2). Fewer than one in 10 citizens (8%) get their water from pipes in their dwelling place or compound. A similar proportion (7%) get theirs from public taps, while two in 10 (20%) use other sources, such as water tanks, rivers, springs, and dams.
Urban residents are five times as likely as rural residents to have piped water inside the house or compound (15% vs. 3%) and twice as likely to get water from public taps (10% vs. 5%) (Figure 3). The use of water sources other than piped water systems, public taps, and boreholes/tubewells is twice as common in rural areas as in the city (26% vs. 13%).
Figure 2: Main source of water for household use | Nigeria | 2020
8

Respondents were asked: What is your main source of water for household use?
Figure 3: Main source of water for household use | by urban-rural location | Nigeria | 2020
15 %

Respondents were asked: What is your main source of water for household use?
But access to a sufficient supply of water is not something that Nigerians can take for granted. A majority (57%) say they went without enough clean water for household use at least once during the year preceding the survey, up from about four in 10 reported in 2014 and 2017 (Figure 4). That includes four in 10 respondents (41%) who experienced water shortages “several times,” “many times,” or “always.” Repeated water shortages were somewhat more common in rural areas (43%) than in the cities (38%).
Figure 4: Went without enough clean water at least once | Nigeria | 2012-2020

Respondents were asked: Over the past year, how often, if ever, have you or anyone in your family gone without enough clean water for home use? (% percentage who said “just once or twice,” “several times,” “many times,” or “always”)
Access to sanitation services
When it comes to access to toilets or latrines, seven in 10 Nigerians (70%) say they have theirs inside the house or compound (Figure 5). But three in 10 (30%) either do not have access to latrines at all or access them outside their compound, a 7-percentage-point increase since 2014 (23%). The poorest citizens (those experiencing high lived poverty[1]) are twice as likely as the economically well-off (those with no lived poverty) to use latrines outside the compound or to lack access to latrines altogether (34% vs. 18%). This situation is three times as common among rural residents (42%) as it is among urban folk (14%) (Figure 6).
Figure 5: Location of toilet or latrine for home use | Nigeria | 2014-2020
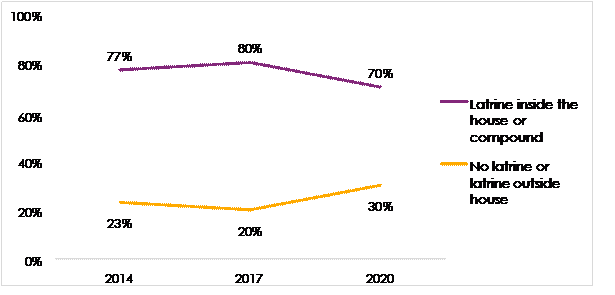
Respondents were asked: Do you have a toilet, water closet, or latrine available for your use? [If yes:] Is it inside your house, inside your compound, or outside your compound, or is there none available?
Figure 6: No toilet or latrine in the compound | by rural-urban location and lived poverty | Nigeria | 2020

Respondents were asked: Do you have a toilet, water closet, or latrine available for your use? [If yes:] Is it inside your house, inside your compound, or outside your compound, or is there none available? (% who say “outside the compound” or “no latrine”)
Access to health care
While access to water and sanitation is a problem for many Nigerians, even more (two-thirds, or 65%) say they went without needed medical care at least once during the previous year, a 22-percentage-point increase since 2014 (Figure 7). For more than four in 10 (44%), this happened “several times,” “many times,” or “always.”
However, among those who had contact with a public clinic or hospital during the previous year, a majority (62%) say they found it “easy” or “very easy” to obtain the care they needed. Even so, a significant proportion (38%) report difficulties in accessing health care, a finding that has been fairly consistent since 2012 (Figure 8).
And two in 10 (21%) of those who sought health care at a public facility say they had to pay a bribe, a troubling finding that has also been fairly consistent over the past four survey rounds (Figure 9).
Figure 7: Went without medical care at least once | Nigeria | 2014-2020

Respondents were asked: Over the past year, how often, if ever, have you or anyone in your family gone without medicines or medical treatment? (% who say “just once or twice,” “several times,” “many times,” or “always”)
Figure 8: Ease or difficulty of obtaining medical care | Nigeria | 2012-2020

Respondents who said they had contact with a public clinic or hospital during the previous year were asked: How easy or difficult was it to obtain the medical care you needed? (Note: Figure excludes those who had no contact with a public clinic or hospital.)
Figure 9: Paid a bribe to obtain medical care | Nigeria | 2012-2020

Respondents who said they had contact with a public clinic or a hospital during the previous year were asked: And how often, if ever, did you have to pay a bribe, give a gift, or do a favour for a health worker or clinic or hospital staff in order to get the medical care you needed? (% who say “once or twice,” “a few times,” or “often”) (Note: Figure excludes those who had no contact with a public clinic or hospital.)
Assessment of government performance
Over the years, approval ratings for the government’s performance in handling water and sanitation and health services have generally been low, and in 2020 they fell lower. Only about a quarter of citizens (27%) say the government is doing “fairly well” or “very well” in providing water and sanitation services, a 13-percentage-point decline after approval had climbed to 40% in 2017 (Figure 10).
And only about one-third (36%) say the government is doing a good job of improving basic health services, a significant decline compared to the previous three rounds of surveys (47%51%).
Figure 10: Approval of government performance in providing water/sanitation services and improving basic health care | Nigeria | 2012-2020

Respondents were asked: How well or badly would you say the current government is handling the following matters, or haven’t you heard enough to say? (% who say “fairly well” or “very well”)
Conclusion
Afrobarometer’s Round 8 survey in early 2020 shows that Nigerians expect better delivery of water/sanitation and health-care services by their government. Approval ratings for the government’s performance in these areas, already low, have declined further. And a majority of citizens say they went without needed medical care and clean water at least once during the previous year, a significant increase compared to 2017.
To effectively fight the COVID-19 pandemic, there is an urgent need for government action and help from all stakeholders, including the private sector, to address gaps in the health sector as well as water and sanitation service delivery.
References
Anadolu Agency. (2020). Nigeria doctors on strike over coronavirus allowance. 1 September.
Premium Times. (2020). Many households lack enough water, soap for handwashing – NBS. 15 July.
Pulse Nigeria. (2020). Impact of COVID-19 on access to quality healthcare for vulnerable populations in Nigeria. 25 August.
Mattes, R. (2020). Lived poverty on the rise: Decade of living-standard gains ends in Africa. Afrobarometer Policy Paper No. 62.
National Bureau of Statistics. (2020). Nigeria – COVID-19 national longitudinal phone survey 2020, Round 3.
Raphael Mbaegbu is the head of social research at NOIPolls, the Afrobarometer National Partner, in Abuja, Nigeria. Email: rmbaegbu@noi-polls.com.
Chukwudebe Nwanze is a senior research associate at NOIPolls. Email: dnwanze@noipolls.com.
Afrobarometer, a nonprofit corporation with headquarters in Ghana, is a pan-African, nonpartisan research network. Regional coordination of national partners in about 35 countries is provided by the Ghana Center for Democratic Development (CDD-Ghana), the Institute for Justice and Reconciliation (IJR) in South Africa, and the Institute for Development Studies (IDS) at the University of Nairobi in Kenya. Michigan State University (MSU) and the University of Cape Town (UCT) provide technical support to the network.
Financial support for Afrobarometer Round 8 has been provided by Sweden via the Swedish
International Development Cooperation Agency, the Mo Ibrahim Foundation, the Open Society Foundations, the William and Flora Hewlett Foundation, and the U.S. Agency for International Development (USAID) via the U.S. Institute of Peace.
Donations help Afrobarometer give voice to African citizens. Please consider making a contribution (at www.afrobarometer.org) or contact Bruno van Dyk (bruno.v.dyk@afrobarometer.org) to discuss institutional funding.
[1] Afrobarometer’s Lived Poverty Index (LPI) measures respondents’ levels of material deprivation by asking how often they or their families went without basic necessities (enough food, enough water, medical care, enough cooking fuel, and a cash income) during the preceding year. For more on lived poverty, see Mattes (2020).

